CLEFT LIP AND PALATE SURGERY
Centre of excellence in Cleft Lip and Palate Surgery in India
Balaji Dental and Craniofacial Hospital is world renowned for its successful cleft lip and palate surgery. It has gained global recognition as a centre of excellence in cleft lip palate surgery and rehabilitation. Cleft lip and palate repair is usually done by a cleft repair specialist/ plastic surgeon. Eminent Maxillofacial Surgeon Prof. Dr. S.M. Balaji adopts advanced concepts and revolutionary innovations in cleft surgery with immense success.
Dr. SM Balaji is one of the best cleft lip surgeons in India. He also excels at cleft palate surgery and is considered to be one of the best cleft palate surgeons.
The hospital receives and serves patients not only from India but also from various parts of the world.
What is Cleft Lip and Palate
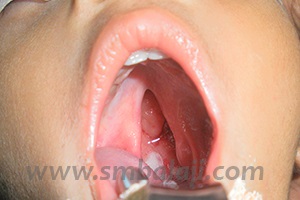
Cleft lip and palate are facial birth deformities. A cleft lip is a gap or discontinuity in the upper lip. A cleft palate is an opening in the roof of the mouth, which divides the mouth and nose. Clefts result from incomplete development of the lip and/or palate in the early weeks of pregnancy. It is during this time that the face is being formed. Separate plates of bone and tissue gradually move towards each other and join to form the lip and palate. When these parts do not join completely, it results in a cleft.
Cleft lip and palate are the most common facial malformations. About 1 in every 700 live births is born with a cleft lip or palate. This accounts for nearly half of all craniofacial anomalies according to the World Health Organization: WHO. Prevalence of cleft lip and palate is based on ancestry.
Dr. SM Balaji is one of the best cleft lip surgeons in India. He also excels at cleft palate surgery and is considered to be one of the best cleft palate surgeons.
The hospital receives and serves patients not only from India but also from various parts of the world.
Prevalence of Cleft Lip and Palate
Prevalence of cleft lip and palate is based on ancestry. It varies among different populations. The highest incidence rate is among the Asian population. The Caucasians have an intermediate prevalence rate. The lowest prevalence rate is among the African population. The prevalence of clefts in India is considerably high when compared to other countries in the world.
Occurrence of Cleft Lip and Palate
The occurrence of cleft lip and palate ranges from 3.4–22.9 per 10,000 births. Cleft lip ranges from 9.92 to 10.8 per 10,000 births. 1.3–25.3 per 10,000 births for cleft palate. India is the second most populated country in the world. It has an estimated population of 1.21 billion people. The estimated occurrence of clefts is about 27,000-33,000 births per year.
Cleft Lip and Palate in Children
Cleft lip also known as harelip refers to an opening or slit in the upper lip. Cleft lip can occur with or without cleft palate and vice versa. Cleft palate refers to a hole in the roof of the mouth. Cleft palate can also occur with or without cleft lip. Unilateral and bilateral clefts usually involve the alveolus of the maxillary arch. Such defects are known as alveolar cleft defect. It can also be unilateral or bilateral.
Classification of Cleft Lip and Palate
Cleft lip can be incomplete cleft lip, unilateral cleft lip or bilateral cleft lip.
Cleft palate can also divided into
Causes of Cleft Lip and Palate
The most common causes of cleft lip and palate are genetic and environmental factors. Clefts are known to occur due to folic acid deficiency, iron and iodine deficiency. It can also occur due to stress.
Environmental factors includes maternal exposure to smoking, use of tobacco, illicit drugs or alcohol consumption during pregnancy. Certain medications like steroids or those prescribed for seizures, cancer, arthritis, tuberculosis etc. Increase in drug dosages. Women taking oral contraceptive pills unaware of their pregnancy.
Exposure to certain viruses or infectious diseases like measles during the developmental stage of the fetus. Exposure to harmful chemicals, vapours, pesticides, gunpowder fumes, nuclear radiation, X-rays, gamma rays or dangerous reagents like in industrial workplaces have hazardous effects.
Genetic occurrence is mainly due to consanguious marriage. Genes responsible includes growth factors like TGFα(8), TGFβ3(14,15) and transcription factors like MSX1, IRF6, TBX22
Treatment timeline of Cleft Lip and Palate
Surgical correction of cleft lip and palate is very essential in the early stages of life. It helps to overcome the feeding difficulty. Various surgical procedures are performed at different stages of life.
What is Cleft Lip Surgery – Cheiloplasty
The main concern in children born with clefts is creating a lip seal to enable to suck the milk. A feeding plate may be given to prevent aspiration of milk through the nose. Specially designed feeding bottles may also be used to help in feeding until 3 months of age. The baby should be held in a 45 degree angulation while feeding to prevent aspiration.
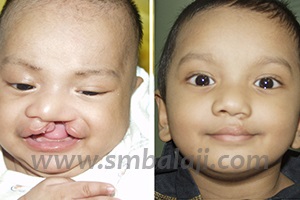
The cleft lip surgery (Cheiloplasty) is done at the age of 3 months. Unilateral cleft lip repair is done using Modified Millard’s technique. Bilateral cleft lip repair is done using Paul Black’s technique. The natural shape of the upper lip is re-created in the best cleft lip and palate hospital in India.
What is Cleft Palate Surgery – palatoplasty
The cleft palate repair surgery (palatoplasty) is performed at about 9 months of age. The cleft palate surgery is done using Veau Wardill Kilner’s technique. It is done to close the gap in the roof of the mouth. Thus creating a barrier between the mouth and the nose.
The palate plays a key role in speech, voice and phonation. This surgery is very essential for normal speech to develop.
What is Pharyngoplasty
Children born with cleft commonly have an increased risk of developing speech problems. They can develop Velopharyngeal insufficiency.
“Velo” refers to the velum, or soft palate. It is the part of the roof of the mouth that moves when you say “ah.”
“Pharyngeal” refers to the throat (pharynx). During normal speech for certain sounds, the palate rises to touch the back of the throat and sends the air out of the mouth.
When a child has VPD, their soft palate does not contact the throat when they talk which lets air escape through their nose during speech. . This leads to a nasal twang in their voice and are difficult to understand.
It is a muscular valve extending from the posterior bony palate to the posterior pharynx. With the exception of /m/, /n/ and /ng/ in the English language all other sounds are produced with a closed velopharyngeal port
Pharyngoplasty combined with speech therapy helps the child to speak well.
Alveolar cleft defect and Premaxillary setback
Alveolar cleft refers to a bone defect in the upper jaw. Protruding pre-maxilla is a characteristic feature of infants with complete bilateral cleft lip and palate. Premaxillary setback along with alveolar cleft defect reconstruction is done to form on single upper jaw. Closure of the cleft in the upper jaw is required to provide a solid surface for the permanent teeth to erupt.
The gap in the upper alveolus can be closed using autograft or alloplast. Autograft is obtained from the child’s hip bone. It may result in a scar in the hip region. RhBMP-2 is an alloplast which can also be used to treat alveolar cleft defect. Nasal and palatal fistula can also be surgically repaired at this stage.
Bone morphogenetic protein 2 – rhBMP2
The use of bone morphogenetic protein-2 (rhBMP-2) bone graft material at our hospital avoids the need to harvest a bone graft from the hip. The synthetic rhBMP-2 stimulates new bone formation by the body’s own cells. This enables new bone growth at the site. Normal teeth eruption and teeth alignment can be achieved.
Additional surgery to harvest bone and subsequent scarring is prevented. Post-surgery recovery is faster and hospital stay is minimum. RhBMP-2 allows earlier alveolar bone grafting treatment at 3.5-4 years of age. Patients previously had to wait until 7.5-8 years to undergo conventional bone graft placement.
However there is considerable variation in the cost of cleft surgery when using autograft and alloplast.
Cleft Orthodontics
A cleft can produce a variety of dental problems. The cleft displaces the teeth; teeth erupt in abnormal positions, disturbing their alignment.
Since children with clefts may have special problems related to missing, malformed, or malpositioned teeth, they require early evaluation by an orthodontist who is familiar with the needs of the child.
Cleft Rhinoplasty | Nose Correction
Children with clefts require the attention of various medical experts and dental experts. Nose correction is an elective surgery and can be done to improve aesthetics. In case of bilateral cleft lip and palate Abbe flap technique is used.
