What is Pharyngoplasty and Why is it Important?
Pharyngoplasty is a surgical procedure to improve the closure of the velopharyngeal (VP) port. The VP port is a muscular valve that separates the oral and nasal cavities. It plays a vital role in eating, breathing, and speech.
When the VP port does not close properly, it can lead to a variety of problems, including:
- Hypernasality: Nasal-sounding speech
- Nasal air emission: Air escaping through the nose during speech
- Velopharyngeal insufficiency (VPI): A condition that can cause difficulty eating, breathing, and speaking
Pharyngoplasty can help to improve or eliminate these problems by correcting the underlying cause of VPI.

How Does Pharyngoplasty Work?
Pharyngoplasty involves repositioning tissue in the throat and mouth to create a stronger and more effective VP port. The specific procedure used will vary depending on the individual’s needs.
Some common pharyngoplasty procedures include:
- Sphincter pharyngoplasty: This procedure involves tightening the muscles of the VP port.
- Pharyngeal flap: This procedure involves creating a flap of tissue from the back of the throat and attaching it to the palate to close the gap between the two structures.
Benefits of Pharyngoplasty
Pharyngoplasty can offer a number of benefits, including:
- Improved speech clarity
- Reduced nasal air emission
- Easier eating and swallowing
- Improved breathing
- Increased self-confidence
Who is a Candidate for Pharyngoplasty?
Pharyngoplasty is typically recommended for people with VPI who have not responded to other treatments, such as speech therapy. It may also be recommended for people with sleep apnea or other breathing problems caused by VPI.
Velopharyngeal Insufficiency
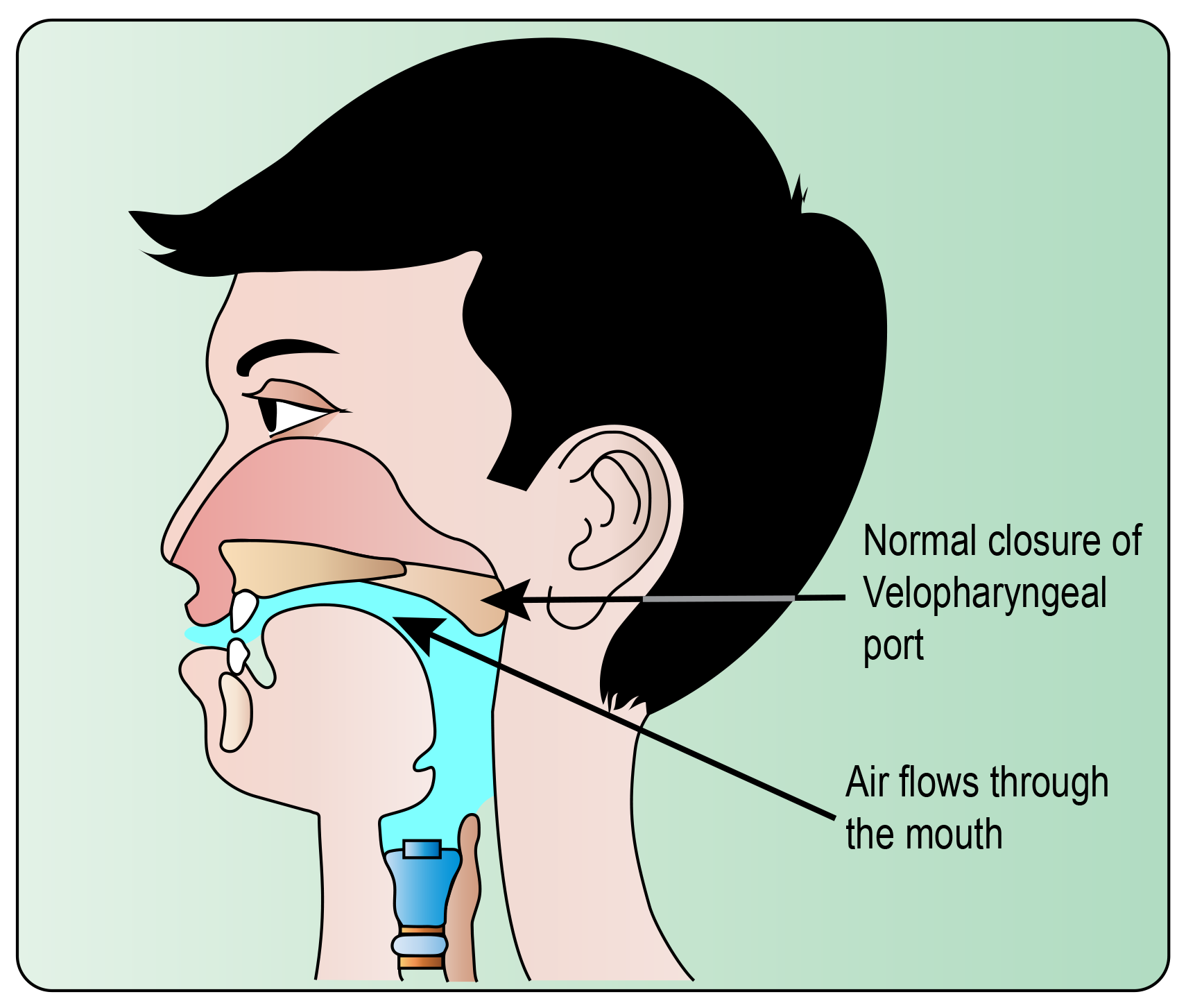
“Velo” refers to the velum, or soft palate. It is the part of the roof of the mouth that moves when you say “ah.”
“Pharyngeal” refers to the throat (pharynx). During normal speech for certain sounds, the palate rises to touch the back of the throat. Thereby sending the air out of the mouth.
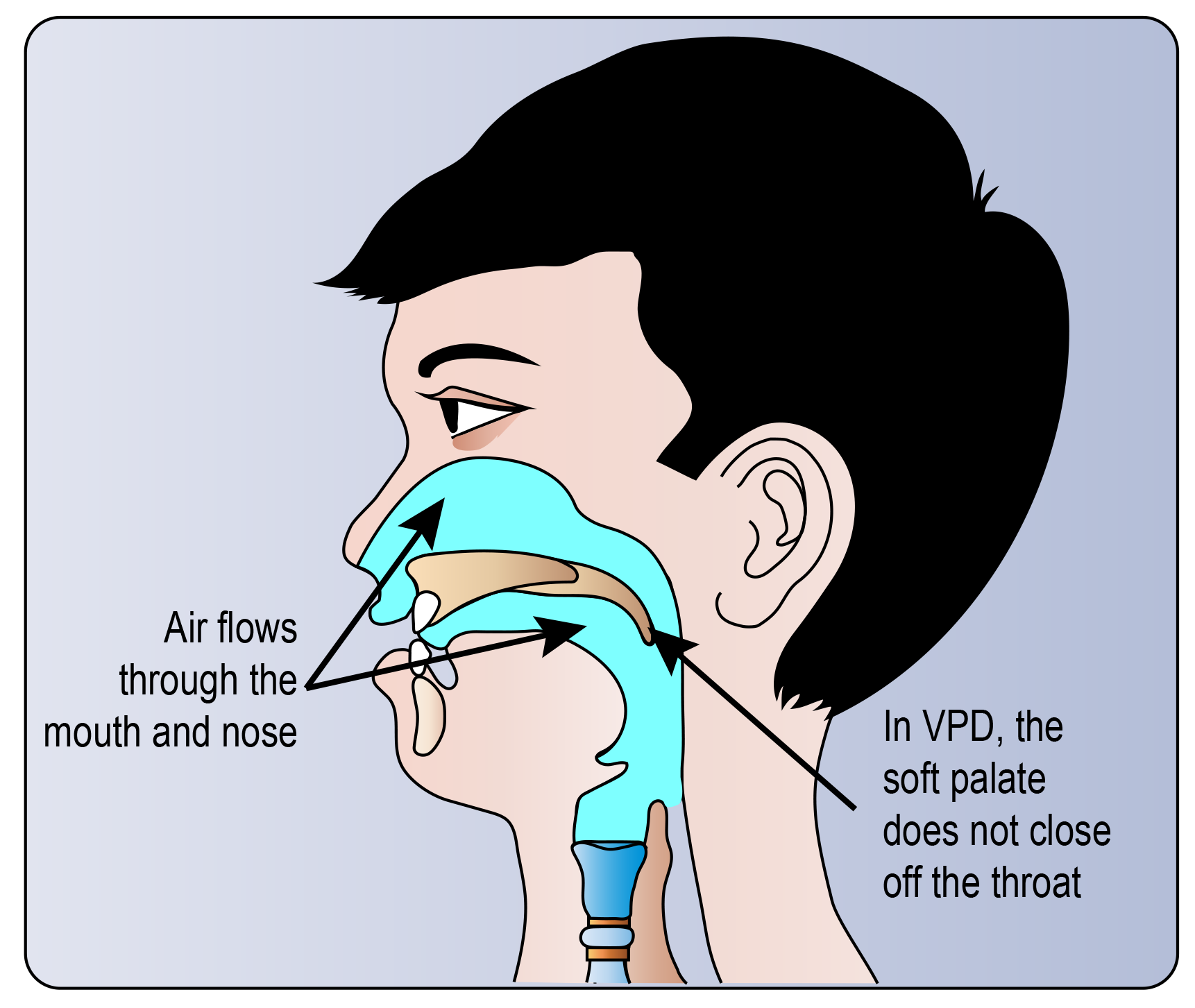
When a child has VPD, their soft palate does not contact the throat during speech. This lets air escape through their nose during speech.
It is a muscular valve extending from the posterior bony palate to the posterior pharynx. Majority of the sounds are produced with a closed velopharyngeal port.
VPI is usually considered as a symptom to velo-cardio-facial syndrome (VCFS).
Occurrence
The occurrence of velopharyngeal dysfunction in India and other countries is due to
- Repaired or unrepaired cleft palate
- Inadequate lengthening of the velum during primary palatoplasty
- Abnormal function of the laevator musculature and cicatricial contracture of the velum
- Submucous clefts
- Neurogenic VPI
– Damage to the cranial nerves innervating the velopharyngeal mechanism
- Genetic conditions.
- Iatrogenic VPI
– Adenoidectomy
– Maxillary resection
– Uvulopalatopharyngoplasty
- Increased space between the palate and the throat.
- Motor speech disorder.
- Unknown causes.
Methods of assessment
Speech language pathologist assesses the velopharyngeal dysfunction.
The Pittsburgh weighted speech score (PWSS) is a standardized scoring system. McWilliams and Phillips described the Pittsburgh weighted speech score (PWSS) in 1979. This tool serves to grade VPI on a quantitative scale. The patients are then classified into four categories of velopharyngeal function. They are
- Competence
- Borderline competence
- Borderline incompetence
- Incompetence
A PWSS score of 3 or greater indicates velopharyngeal incompetence.
Closure patterns
The closure patterns of the Velopharyngeal port are of 3 types. It is based on the movements of the velum and the pharyngeal walls (posterior pharyngeal wall).
- Circular/Constricted: Combined movements of the velum and pharyngeal walls contribute equally to close the port in a “purse-string” fashion.
- Coronal: Posterior and superior movement of the velum is primarily responsible for velopharyngeal closure, with little contribution from the lateral pharyngeal walls.
- Sagittal: Medial displacement of the lateral pharyngeal walls which is primarily responsible for closure, with little posterior movement of the velum.
Methods to assess closure patterns
The recommended age for surgical procedure depends on the clinical problem. The child’s speech is to be clearly observed. This is important in case of children with cleft. Surgical recommendations are only made after evaluation. The evaluation is usually done by a trained speech therapist.
For assessment the child has to be 3 and 1/2 to 4 years old. Children over 4 years co-operate better to speech evaluation. The hypernasality correction is to be done before kindergarten or first class. This is the age when children begin noticing differences. Pharyngoplasty must be done before the brain gets accustomed to the speech.
An alternative option is the use of a removable dental appliance. This fills the gap in the back of the throat. This also prevents excess air leakage from the throat during speech. This appliance is designed by a speech Prosthodontist.
The methods for studying the closure pattern of velopharyngeal port are:
- Nasoendoscopy (NE) – A flexible endoscope is used to provide a bird’s eye view. The location, shape and size of the opening can be determined. It is also used to assess palatal scarring.
- Multiview Video Fluoroscopy (MVF) – It is a non-invasive procedure. It refers to images that are obtained during speech. The contribution of the velum and lateral pharyngeal walls to velopharyngeal closure can be determined.
- Magnetic Resonance Imaging (MRI)- MRI is non-invasive. It is commonly used in un-cooperative patients. It is also used where precise anatomical information is necessary.
- Nasometry- It is a device used to measure the energy emitted during speech. It is a very sophisticated device and is attached to a computer. The results are noted as nasalance score. It is purely objective but still used as a adjunct to speech development.
Pharyngoplasty in India – Surgical techniques
The surgical management varies from person to person
- Sphincter pharyngoplasty
- Furlow’s pharyngoplasty
- Pharyngeal flap
- Posterior pharyngeal wall implant
During surgery the VPI port is reduced to a small gap. Thereby preventing air from escaping through the nose. Thus creating a positive pressure.
Patients who require usually have nasal twang. Long term speech difficulties can be corrected by pharyngoplasty. Pharyngoplasty is considered to come under plastic surgery. As a result it is usually done by a plastic surgeon. It can also be done by a pharyngoplasty specialist. Pharyngoplasty does not lead to obstructive sleep disorders.
Furlow’s pharyngoplasty
It is also known as Z-plasty. Furlow’s pharyngoplasty is a plastic surgical technique. It involves lengthening and thickening the soft palate. Along with realignment of abnormally placed palatal muscles. This operation is usually performed for children with clefts. Hypernasality may occur even after cleft palate repair.
It can also occur in patients with a hidden cleft palate. The increase in thickness and length provides improved contact. Thus preventing air leakage from the nose during speech. This procedure is also known to be beneficial in cleft palate patients with ear infections.
Sphincter pharyngoplasty
Sphincter pharyngoplasty refers to raising layers of muscle from the throat. The muscle is dissected from behind the tonsil. It is later folded over each other. Then sewn together side to side. This ridge of muscle acts like a bump in the back of the throat.
Thus enabling the palate to rise up during speech. The size of the muscle dissected is based on the child’s anatomy (i.e. the shape and size of the gap located in the throat). This muscle layer cannot be visualized after surgery.
This procedure is more preferable than other types of pharyngoplasty. There are less chances of post-operative airway obstruction. The in-hospital recovery time is also less. The recovery period is about one night only.
Sphincter pharyngoplasty is followed in the best VPI correction hospital in India. Balaji Dental and Craniofacial Hospital is one of the best center for cleft lip and palate surgery in India. Some of the best palate surgeries are done here. The cost is also less when compared to other hospitals.
Pharyngeal flap technique has a recovery period of about 3-5 nights.
Conclusion
VPI is a common complication following palatoplasty. The selection of operative procedures depends on the multimodal patient assessment. It includes speech evaluation and imaging studies of the pharyngeal mechanism.
A thorough understanding of the velopharyngeal anatomy and its physiology is crucial. This helps in understanding the deficit in patients with VPI. The success rate varies from 85-98% depending on the age.
Pharyngoplasty can also be done in older patients. Depending on the age the success rates varies. The success rate is about 60%-85% in patients who are about 35-40 years of age.